Insulin resistance testing can offer several benefits in clinical practice. It not only helps diagnose insulin resistance in the early stages but can also help monitor progression and assess the effectiveness of treatment. By identifying insulin resistance in the early stages with testing, healthcare providers can recommend lifestyle changes, including dietary recommendations, exercise interventions, and stress management techniques that can help improve insulin sensitivity and prevent further disease progression. By preventing further progression, patients can also decrease the chances they will need medications in the future to control their blood sugar.
Testing can be beneficial in patients with conditions associated with insulin resistance, such as Polycystic ovarian symptoms, Hashimoto’s disease, obesity, cardiovascular disease and metabolic syndrome. Insulin resistance can also occur in pregnancy; therefore, routine insulin testing during this time can be beneficial for preventing the onset and progression of gestational diabetes.
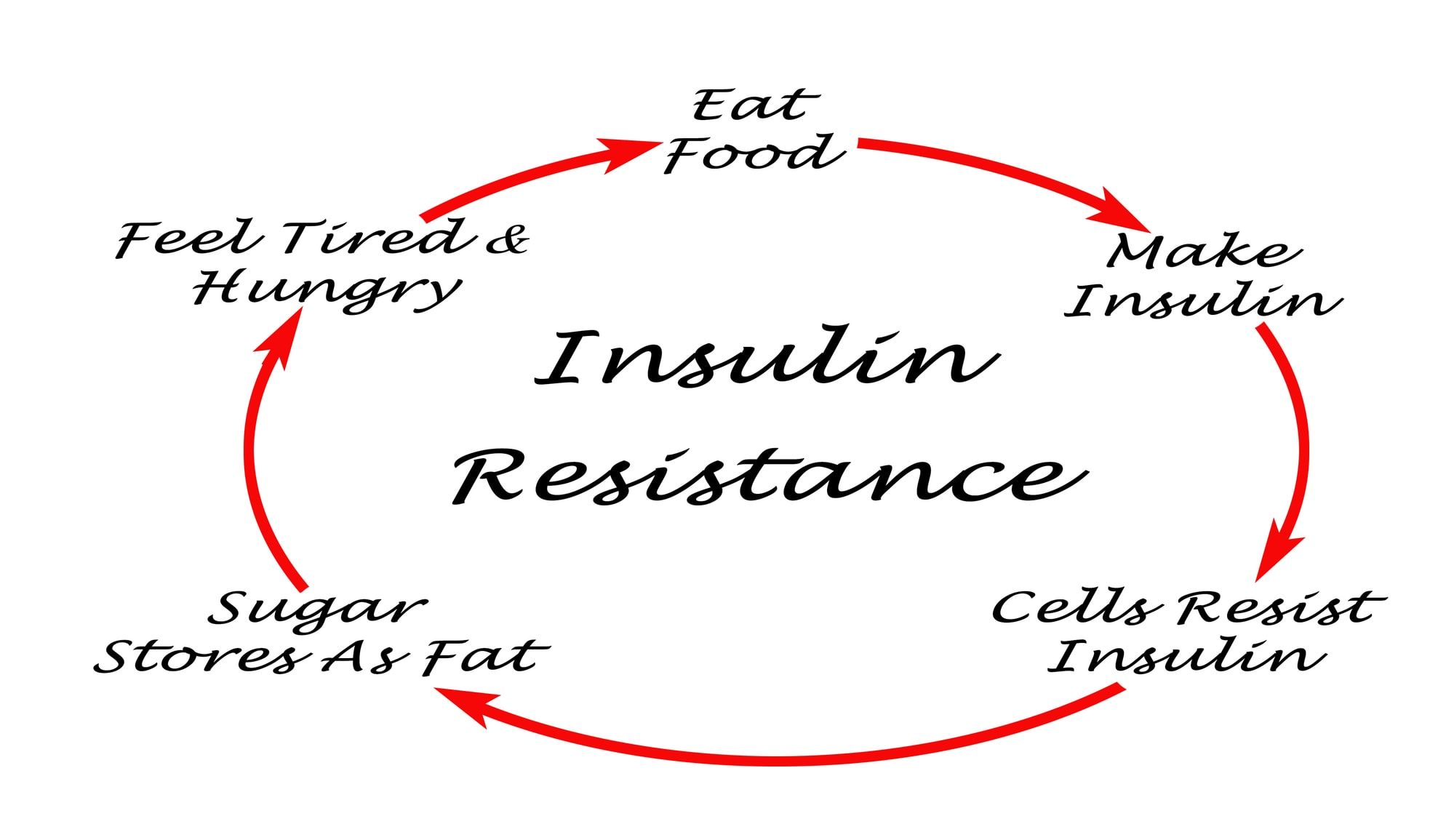
What is Insulin Resistance?
Insulin is a hormone the pancreas produces that allows cells to uptake glucose from the blood for energy. Insulin resistance occurs when cells throughout the body do not adequately respond to insulin and, therefore, can not utilize the glucose in the blood. Due to this, the pancreas secretes more insulin to lower blood sugar levels. The constant high levels of insulin further desensitize cells to the effects of insulin. Over time, this leads to not only chronically high levels of insulin but also elevated blood sugar levels. Insulin resistance is assessed by several tests, including evaluating how much insulin is in the bloodstream after prolonged periods of fasting.

What are the symptoms of Insulin Resistance?
Insulin resistance means that cells cannot utilize glucose, leading to dysfunction of cells. This can lead to symptoms such as:
- Low energy/ fatigue: due to the cell’s inability to use glucose, their primary fuel source.
- Increased thirst and frequency of urination: high blood sugar levels due to insulin resistance can cause increased thirst and urination.
- Weight gain or weight loss resistance: insulin resistance is associated with weight gain, particularly in the abdominal area.
- Increased hunger and food cravings: Insulin resistance is implicated in appetite dysregulation. This can often lead to increased hunger, frequently accompanied by cravings for sweet or high-carbohydrate foods.
- Skin changes: skin changes may occur, including darkened patches of skin. These are most common on the neck, armpits and other skin folds. A common skin change seen in those with poor insulin function is acanthosis nigricans.
- Weak immune system: Insulin resistance can lead to impaired immune function, resulting in frequent infections and poor wound healing.
What is the difference between Insulin Resistance and Prediabetes?
While prediabetes is often caused by insulin resistance, they are not the same. Prediabetes and type 2 diabetes occur when the pancreas does not make enough insulin to support proper blood sugar management. Insulin resistance occurs when there is sufficient or abundance of insulin, but the cells do not respond to insulin. Ultimately, the pancreas secretes so much insulin that the cells that produce insulin start to wear out. This can eventually lead to lower levels of insulin seen in prediabetes and diabetes.
What are risk factors for insulin resistance?
Both lifestyle factors and genetics can increase a person’s risk of developing insulin resistance. Some risk factors include:
- Obesity/ being overweight
- A parent or sibling with diabetes
- Physical inactivity/ sedentary lifestyle/ lack of exercise
- High-stress levels
- Poor sleep/ sleep deprivation
- Hormonal dysregulation
- High carbohydrate diet/ high sugar diet
- A history of gestational diabetes
- High blood pressure, cardiovascular disease, heart disease
- Thyroid cancer/ Damage to the thyroid gland’
- Prolonged dysregulation of hormones
What Tests Can Be Used to Evaluate Insulin Resistance?
Various tests are used to evaluate the body’s ability to utilize insulin. All of the tests evaluate different processes in the body. Oftentimes, a combination of tests will be used to determine the current function of the individual’s blood glucose control and best guide treatment.
The Fasting Plasma Glucose (FPG) Test
Measures blood sugar levels after at least 8 hours of fasting. After fasting for this long, blood sugar levels should be low. Increased blood sugar levels while fasting can indicate early signs of insulin resistance.
Oral Glucose Tolerance Test (OGTT)
This test involves the administration of a high-sugar beverage and subsequent measurements of blood sugar levels. It evaluates an individual’s response to regulating blood sugar levels after a high sugar intake.
Hemoglobin A1c (HbA1c) Test
Is one of the most common tests to evaluate blood sugar control. It measures the amount of glucose attached to red blood cells. This is useful for assessing an individual’s average blood sugar levels over the past 2-3 months.
Fasting Insulin Test
Similar to fasting glucose, fasting insulin levels show the amount of insulin in the blood after a prolonged fasting period. High levels of insulin, particularly when paired with elevated fasting glucose levels, can indicate insulin resistance.
C-Peptide Test
C peptide is a marker that your body produces insulin. A high C peptide may indicate that your body is producing large amounts of insulin, commonly seen in insulin resistance. A low C- peptide may suggest that your body has little or no insulin, which is widely seen in prediabetes and diabetes.
HOMA-2 (HOMA IR) Test
This test is a calculation that helps to estimate an individual’s degree of insulin sensitivity. It uses measurements from fasting blood sugar, fasting insulin and C-Peptide.
Triglycerides Test
insulin also allows the body to use triglycerides for energy. High triglycerides are often seen in those with high carbohydrate diets. A high level of triglycerides can indicate insulin resistance.
Cholesterol Test
Abnormal cholesterol levels are often seen in those with insulin resistance. Due to insulin resistance, individuals can develop low levels of HDL (good cholesterol) or high levels of LDL (bad cholesterol).
Why Is It Important to Test for Insulin Resistance?
There are many reasons testing for insulin resistance is important. Even without significant signs and symptoms, insulin resistance may be present.
Reasons for testing for insulin resistance include:
Early detection
Insulin resistance is often a precursor to more severe conditions such as diabetes and prediabetes. Insulin resistance and the early stages of these conditions may not always have obvious symptoms. Due to this, testing can help identify the presence of insulin resistance, even if there are no significant symptoms.
Treatment guidance
Using many tests can allow for the best evaluation of what is going on in a patient’s body. This helps providers curate a personalized treatment plan to address the patient’s needs best. This will yield superior results compared to generalized treatments.
Risk assessment
Insulin resistance is associated with several other conditions, including, but not limited to, diabetes, cardiovascular disease, metabolic syndrome, high blood pressure/ hypertension, and polycystic ovarian syndrome (PCOS). Utilizing a wide range of testing can assess an individual’s risk of developing these conditions.
Monitoring treatment progress
Routine testing can help evaluate the effectiveness of treatment and help indicate if adjustments to the treatment protocol are needed.
Prevention
Insulin resistance is often an early sign of dysfunction. Therefore, early testing and diagnosis can help prevent further progression and improve health outcomes.
What Other Conditions Are Associated With Insulin Resistance?
Several conditions are associated with insulin resistance. Some of these conditions are caused by insulin resistance or may cause insulin resistance. Having one or more of these conditions may mean that insulin resistance testing may be indicated for you.
- Prediabetes/ diabetes
- Metabolic syndrome/ obesity
- Cushing’s syndrome/ Cushing’s disease
- Cardiovascular disease
- Polycystic Ovarian Syndrome
- Hypothyroidism/ dysfunction of thyroid hormone
- Liver disease/ fatty liver disease
- Heart disease
- Stroke
- Depression
- Hyperthyroidism/ thyroiditis
Women entering and transitioning through menopause also experience metabolic and hormonal changes that increase their risk for insulin resistance. Due to this, insulin resistance testing may be indicated in women transitioning or who have entered menopause.
Find out how a Naturopathic Doctor can help with Insulin Management
Frequently Asked Questions About Insulin Testing
How Much Does Testing Cost?
Test prices vary depending on what specific tests are indicated and used. A full link to testing prices can be found on the fees page.
How Long Does Testing Take?
Most tests assessing insulin resistance and metabolic function use a simple blood draw. This process usually only takes a few minutes. Many of the tests require 8-14 hours of fasting before going to the lab location. Test results are usually received within a few days of testing but can vary based on location.
How To Know When To Get Tested?
Working with your naturopathic doctor will allow you to determine if testing and evaluation for insulin resistance is indicated for you. Naturopathic doctors use clinical symptoms, patient history and other diet and lifestyle factors to determine if you are at risk or are showing signs and symptoms of insulin resistance.
What Happens After Your Test?
After the blood work results return, a Naturopathic Doctor or other health care provider can interpret the results and decide the next best steps.


